This article was automatically translated from the original Turkish version.
+2 More
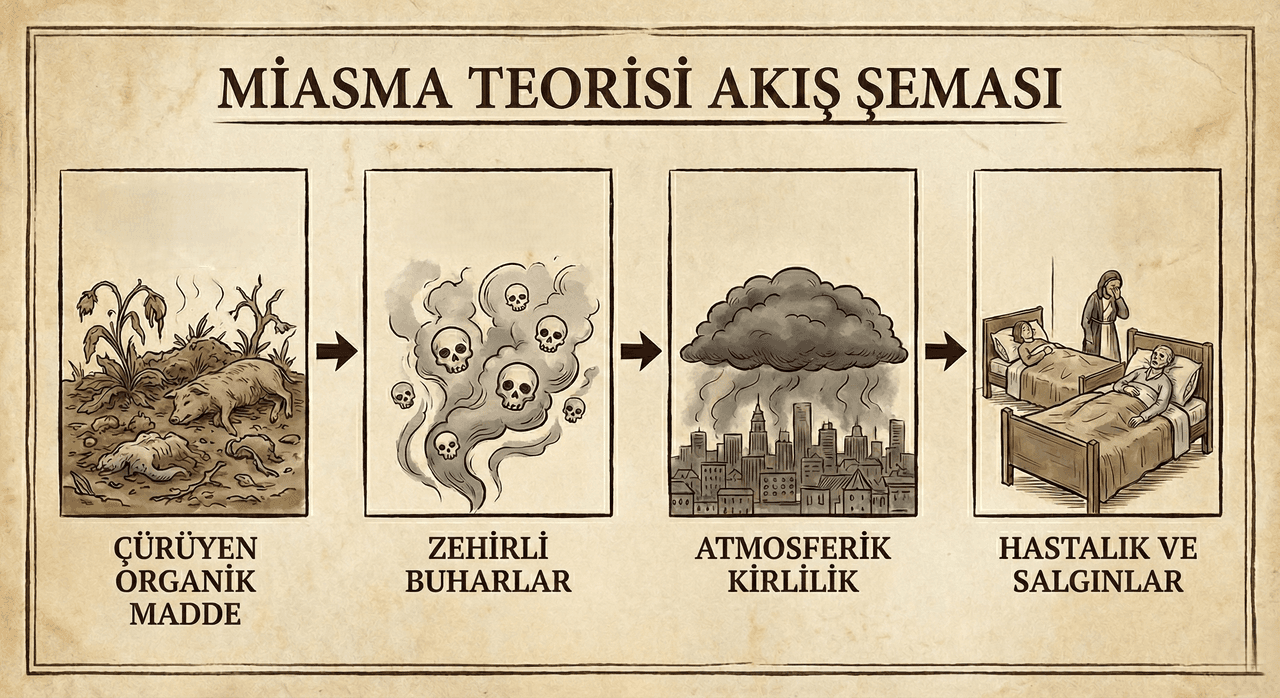
The miasma theory is a medical approach that attributes the origins of epidemics and general health problems to poisonous vapors emitted by decaying organic matter, swamps, stagnant waters, or unsanitary environmental conditions that pollute the atmosphere. According to this concept, diseases arise not from specific microscopic agents but from the degradation of the quality of the air surrounding individuals. The theory asserts that “atmospheric pollution” plays a decisive role in disease formation, particularly claiming that gases produced by the decomposition of animal and plant matter in crowded, humid, and poorly ventilated areas threaten human health.

Representative Image Depicting the ‘Bad Air’ and Foggy Atmosphere Believed to Be the Source of Disease According to the Miasma Theory. (Generated by Artificial Intelligence.)
When examined conceptually, miasma is defined not merely as a bad odor but as the direct effect of environmental factors on the human body. From this perspective, seasonal changes, wind direction (hot or cold), the nature of water sources (swamp, rainwater, or hard water), and soil composition determine the physical characteristics and disease susceptibility of populations in a given region. Thus, illness is not caused by an external agent but is linked to the air individuals breathe and the environmental conditions they are exposed to.
Within the miasma framework, the concept of “infection” is not understood as direct transmission from person to person but as the loss of air purity and the increase in contamination. According to this view, air in enclosed and poorly ventilated spaces becomes corrupted due to the effects of sewage fumes or decaying matter, and this corrupted air “reproduces” disease. The fundamental condition for recovery and health preservation is maintaining the ambient air as pure as outdoor air, ensuring adequate light, and eliminating moisture from the environment.
Historically, this theory shaped public health approaches by necessitating environmental interventions—such as the construction of drainage systems, street cleaning, ventilation, and draining of swamps—rather than focusing on quarantine or personal isolation to prevent epidemics.
The intellectual foundations of the miasma theory extend to ancient Greek medicine, which sought to explain disease causes through physical and environmental factors rather than supernatural forces, particularly in Hippocrates’ work On Airs, Waters, and Places. The text emphasizes that anyone seeking to study medicine correctly must examine seasons, winds (hot and cold), water qualities, and the locations of cities【1】. According to this perspective, a region’s atmospheric conditions and geographical structure directly determine the character of diseases occurring there and the physical resilience of its inhabitants.
In the historical development of the theory, the “air” factor plays a decisive role. According to Hippocratic views, a city’s orientation relative to prevailing winds shapes the health of its residents. For example, cities exposed to hot winds (southerly winds) but shielded from northerly winds typically have salty and shallow waters; the inhabitants of such cities tend to have moist and “flaccid” heads. These individuals commonly exhibit increased phlegm and are prone to intestinal disorders. In contrast, cities exposed to cold northerly winds have hard and cold water; their residents possess a more robust, lean, and “bilious” constitution【2】.
Another pillar of environmental determinism is water sources. At the root of the miasma theory lies the belief that stagnant and swampy waters emit “bad air” and cause physical deformities. Communities relying on swampy or stagnant water were thought to have swollen abdomens, enlarged spleens, and generally exhibited a “phlegmatic” (heavy-tempered/calm) constitution. In contrast, waters flowing from rocky areas were considered healthier.
These ancient observations formed the foundation of the miasmatic view, which for centuries linked disease causes to environmental factors and reinforced the belief that diseases arose from harmful vapors rising from soil or water and polluting the atmosphere. As George Rosen noted in his analysis of public health history, this environmental approach removed diseases from the realm of divine punishment and placed them within a rational—though limited by the knowledge of the time—causal framework.【3】
The miasma theory became the most influential doctrine in shaping modern public health policies and urban infrastructure reforms during the 19th century. The concept of “atmospheric pollution” as the primary cause of disease during this period triggered a comprehensive “Sanitary” (Hygienic) movement that demanded engineering and architectural interventions rather than purely medical responses.
In England, the Report on the Sanitary Condition of the Labouring Population, prepared in response to the deplorable living conditions brought by the Industrial Revolution, functions as the bureaucratic manifesto of the miasma theory. In this report by Edwin Chadwick, the source of epidemics is directly linked to environmental factors. According to Chadwick, dampness, filth, and overcrowded housing generate harmful vapors from decaying animal and plant matter. This corrupted atmosphere is the primary cause of febrile illnesses, particularly in impoverished neighborhoods.【4】
In Chadwick’s view, disease is not a phenomenon transmitted from person to person but a consequence of exposure to “bad air.” Therefore, the solution lies not in individual restrictions such as quarantine but in constructing drainage systems, ensuring continuous water flow, removing garbage from streets, and ventilating homes. The report argues, based on the assumption that “all smell is disease,” that eliminating atmospheric pollution would prevent illness【5】.
One of the strongest practical advocates of the miasma theory was Florence Nightingale. In her work Notes on Nursing, Nightingale established the first rule of nursing as maintaining the air breathed by the patient as clean as outdoor air. For her, clean air, light, temperature, silence, and cleanliness were vital for recovery, and their absence intensified illness.【6】
Nightingale approached the era’s prevalent “contagion” theory with skepticism. Rejecting the idea that diseases such as smallpox or measles inevitably spread directly from person to person, she argued that unsuitable environmental conditions could reproduce illness. For her, “infection” was the result of accumulated filth and stagnant air in closed, dark, and poorly ventilated rooms. In this context, opening windows, ventilating rooms, removing dust from carpets, and eliminating sewer odors from living spaces were not merely medical recommendations but necessities.
Although the practices based on the miasma theory could not fully explain biological mechanisms (the germ theory), they played a decisive role in reducing mortality rates and advancing modern urbanism through their focus on hygiene and infrastructure reform.【7】
The miasma theory was one of the key elements shaping public health policies and societal perceptions of disease in the Ottoman Empire during the 19th and early 20th centuries. In particular, during Istanbul’s cholera outbreaks, the belief that the disease originated from “corrupted air” merged with emerging bacteriological knowledge to produce a unique form of resistance practice.
The cholera outbreak in Istanbul during the summer of 1911 demonstrated how deeply entrenched miasmatic thinking remained in public perception. Newspapers of the time, such as Alemdar, frequently attributed the spread of the disease to environmental and psychological factors such as “air change” and “fear”【8】. One article in the newspaper claimed that cholera was not inherently terrifying but that the panic and “fear” experienced by the public intensified the outbreak.
Among the public, it was widely believed that the disease arrived with “air change” and would naturally subside as temperatures cooled. Consequently, efforts to combat the outbreak included not only medical measures but also spiritual and environmental purification rituals. Newspaper columns frequently promoted miasma-based advice such as breathing “clean air,” benefiting from sunlight, and avoiding damp places to prevent disease spread.
Ottoman municipal administration adopted a “sanitary” (hygienist) approach to combating epidemics from the late 19th century onward. This approach largely aligned with the principle advocated by Chadwick in his British report: removing foul odors and filth. During the fifth cholera pandemic, the Ottoman administration launched extensive sanitation campaigns aimed at eliminating the sources of disease through drying and cleaning.

Representative Image Depicting Street Washing and Lime Washing Operations Conducted in the Ottoman Period to Combat Cholera Outbreaks. (Generated by Artificial Intelligence.)
One of the most important measures taken by municipalities was the regular washing and liming of streets. This practice aimed to remove visible filth and prevent harmful vapors believed to rise from the soil. Additionally, “Tebhirhaneler” (disinfection stations) were established to clean suspicious items and clothing using high-temperature steam. Although this “tebhir” (steaming) process signaled a transition toward germ theory, its underlying logic still rested on the idea of eliminating disease-causing elements before they could enter the air.
Moreover, as noted in Alemdar, the Istanbul Municipality intensified measures such as removing garbage piles, improving latrines, and monitoring food sold openly【9】. Particularly during summer months, when rising temperatures increased the odor from decaying matter (watermelon and melon rinds, etc.), strict cleanliness inspections were conducted in marketplaces. These practices demonstrate how the miasma theory in the Ottoman Empire transformed into a practical “environmental cleaning” movement and laid the foundation for modern municipal services.【10】

Caricature from Punch Magazine, 1858, Entitled ‘Baba Thames Presents the Children of London to the City.’ (victorianweb.org)
The scientific questioning and eventual refutation of the miasma theory began in the mid-19th century with epidemiological studies on the transmission mechanisms of cholera. The most important figure in this process was Dr. John Snow, who argued that cholera was not spread through “corrupted air” (effluvia) but via a specific substance.
In his work On the Mode of Communication of Cholera, John Snow rejected the miasma theory’s assumption that disease spread through airborne poisons. Snow argued that if cholera originated from toxic gases in the air, symptoms would first appear in the respiratory system and then enter the bloodstream, causing a generalized poisoning similar to malaria. However, cholera consistently began in the digestive system, first affecting the stomach and intestines before disrupting circulation. This pattern indicated that the disease agent must be sought not in the air inhaled but in a substance ingested.【11】
Snow also analyzed the pattern of disease spread. While miasma proponents attributed simultaneous infections among many people to “atmospheric pollution,” Snow argued that the disease spread from person to person, not through direct contact but through contamination of food or drink by substances excreted by infected individuals. In overcrowded homes of poor families, where handwashing was absent and food was prepared near sickbeds, this “invisible” transmission was facilitated.

Dr. John Snow’s Map Showing Cholera Deaths Around the Broad Street Pump During the 1854 London Outbreak. (wellcomcollection.org)
The severe cholera outbreak in London’s Soho district in 1854 provided one of the key pieces of evidence against the miasma theory. When Snow mapped the deaths in the area, he found that nearly all cases clustered around the public water pump on Broad Street. If the area had truly been contaminated by “bad air,” as miasma proponents claimed, the disease would have spread more widely and according to wind direction. However, Snow demonstrated that individuals who did not drink from the pump (such as workers at a nearby brewery who consumed their own beer) remained unaffected, while those who had moved away from the area but continued drinking its water fell ill.
A broader proof came from an analysis of the two major water companies supplying London: Southwark & Vauxhall and Lambeth. Southwark & Vauxhall drew water from the polluted (sewage-discharging) lower reaches of the Thames River, while Lambeth sourced its water from cleaner, upstream sections. Snow’s statistical analysis revealed that households using contaminated water had dramatically higher cholera mortality rates than those using clean water. This stark difference among residents living in the same neighborhood, breathing the same air, and sharing similar socioeconomic conditions irrefutably demonstrated that the cause of the disease was not “air” (miasma) but “water.”【12】
Although Snow’s work predated the identification of the bacterium Vibrio cholerae, it established that the disease spread through a specific material, thereby undermining the scientific validity of the miasma theory.
The miasma theory was replaced by the “Germ Theory,” whose foundations were laid by the work of Louis Pasteur and Robert Koch, which attributes disease causes not to vague atmospheric disturbances but to specific microorganisms. In modern pathology, infectious diseases are defined as processes resulting from the interaction between host organisms and pathogens such as viruses, bacteria, fungi, and parasites.
According to modern medical science, infectious diseases are not spontaneous disturbances as the miasma theory suggested; rather, they begin when pathogenic organisms enter the body from humans, animals, insect vectors, or the environment. Entry routes for pathogens include the respiratory, digestive (fecal-oral), urogenital systems, or breaches in skin integrity.
The miasma theory’s claim that inhaling “bad air” causes disease finds only partial correspondence in modern medicine, though the mechanism is entirely different. Microorganisms causing respiratory infections (such as influenza viruses or the bacterium responsible for tuberculosis, Mycobacterium tuberculosis) are not transmitted through “corrupted air” but via particles suspended in the air as aerosols or droplets. The body’s natural defense mechanisms (mucociliary clearance, alveolar macrophages) attempt to remove these particles; illness occurs only when these defenses are overwhelmed or the pathogen is highly virulent. Thus, air is not the disease itself (miasma) but a carrier (vector) of the pathogen.
The miasma theory’s observations linking “swamps and hot weather” to disease have been reinterpreted in modern epidemiology within the context of “environmental exposure” and “climate change.” However, this relationship is now explained not by gases emitted from decaying matter but by ecological impacts on pathogens and vectors.
According to Harrison’s Principles of Internal Medicine, climatic conditions directly influence the epidemiology of infectious diseases. For instance, the swamps and wetlands that miasmatic theorists identified as the most polluted areas are in fact breeding grounds for mosquitoes that transmit malaria and dengue fever. Rising temperatures increase the reproduction rate and biting frequency of these vectors, facilitating disease spread.【13】 Similarly, excessive rainfall and flooding cause sewage to mix with water sources, triggering outbreaks of cholera and other waterborne diseases.
Although the miasma theory’s causal mechanism—linking disease to foul odors—has lost its validity today, its focus on environmental conditions (temperature, humidity, pollution) played a decisive role in shaping early public health policies. The measures implemented by reformers such as Chadwick and Nightingale to “remove miasma”—including drainage, ventilation, and cleaning—were theoretically based on a flawed premise but were practically successful because they reduced pathogen load and vector breeding, thereby laying the foundations of modern public health.
"Father Thames Introducing His Offspring to the City of London" (Father Thames Cartoon). *Punch* (July 3, 1858). Source: Victorian Web via Internet Archive and University of California Library. Accessed February 9, 2026. https://victorianweb.org/periodicals/punch/publichealth/4.html
Alıcı, Abdulvahap, and Öner Atay. "Osmanlı Devleti’nde Beşinci Kolera Pandemisi ve Sosyal Belediyeciliğin Salgının Önlenmesine Etkileri." *Medeniyet ve Toplum Dergisi* 8, no. 2 (2024): 283-304. Accessed February 8, 2026. https://dergipark.org.tr/tr/pub/metder/article/1610848
Bernstein, Aaron S., and Jonathan A. Patz. "Climate Change and Infectious Disease". In Harrison’s Principles of Internal Medicine, 22nd ed., edited by Joseph Loscalzo, Anthony Fauci, Dennis Kasper, Stephen Hauser, Dan Longo, and J. Larry Jameson, 3744-3754. New York: McGraw Hill, 2022.
Bingül, Şeyhmus. "Alemdar Gazetesi’ne Göre 1911 Yazında İstanbul’un Kolera ile İmtihanı". *Lokman Hekim Dergisi* 11, no. 1 (2021): 157-168. Accessed February 8, 2026. https://doi.org/10.31020/mutftd.726753
Chadwick, Edwin. *Report on the Sanitary Condition of the Labouring Population of Great Britain*. London: W. Clowes and Sons, 1842. Accessed February 8, 2026. https://wellcomecollection.org/works/j23vgsgx/items.
Frank, Karen M., and Alexander J. McAdam. "Infectious Diseases". In Robbins & Cotran Pathologic Basis of Disease, 10th ed., edited by Vinay Kumar, Abul K. Abbas, and Jon C. Aster, 339-399. Philadelphia: Elsevier, 2021.
Hippocrates. *On Airs, Waters, and Places*. Translated by Francis Adams. The Internet Classics Archive. Accessed February 8, 2026. http://classics.mit.edu//Hippocrates/airwatpl.mb.txt
Nightingale, Florence. *Notes on Nursing: What It Is, and What It Is Not*. New York: D. Appleton and Company, 1860. Accessed February 8, 2026. https://www.gutenberg.org/cache/epub/12439/pg12439-images.html
Rosen, George. *A History of Public Health*. Revised Expanded Edition. Baltimore: Johns Hopkins University Press, 2015. Accessed February 8, 2026. https://saludprevencion.com/wp-content/uploads/2025/05/Rosen-A-History-of-Public-Health.pdf
Snow, John. "Map 1. showing the deaths from cholera in Broad Street, Golden Square, and the neighbourhood." *Report on the cholera outbreak in the Parish of St. James, Westminster, during the autumn of 1854*. Cholera Inquiry Committee, July 1855. Wellcome Collection. Accessed February 9, 2026. https://wellcomecollection.org/works/uxgfjt62/images?id=d4gnqhwy
Snow, John. *On the Mode of Communication of Cholera*. 2nd ed. London: John Churchill, 1855. Accessed February 8, 2026. https://wellcomecollection.org/works/uqa27qrt/items
[1]
Hippocrates. "On Airs, Waters, and Places." The Internet Classics Archive (400 BCE): Part 1-3. Access Date: February 8, 2026. http://classics.mit.edu//Hippocrates/airwatpl.mb.txt.
[2]
Hippocrates, On Airs, Waters, and Places, Part 3-4.
[3]
George Rosen, A History of Public Health, Revised Expanded Edition (Baltimore: Johns Hopkins University Press, 2015), 60-62, Access February 8, 2026, https://saludprevencion.com/wp-content/uploads/2025/05/Rosen-A-History-of-Public-Health.pdf.
[4]
Edwin Chadwick, Report on the Sanitary Condition of the Labouring Population of Great Britain (London: W. Clowes and Sons, 1842), 369-370, Access February 8, 2026, https://wellcomecollection.org/works/j23vgsgx/items.
[5]
Chadwick, Report on the Sanitary Condition, 370-372.
[6]
Florence Nightingale, Notes on Nursing: What It Is, and What It Is Not (New York: D. Appleton and Company, 1860), 8-9, Access February 8, 2026, https://www.gutenberg.org/cache/epub/12439/pg12439-images.html.
[7]
Rosen, A History of Public Health, 205-207.
[8]
Şeyhmus Bingül. "Alemdar Gazetesi’ne Göre 1911 Yazında İstanbul’un Kolera ile İmtihanı." Lokman Hekim Dergisi Vol. 11, No. 1 (2021): 161-162. Access Date: February 8, 2026. https://doi.org/10.31020/mutftd.726753.
[9]
Bingül, "Alemdar Gazetesi’ne Göre," 165.
[10]
Abdulvahap Alıcı ve Öner Atay, "Osmanlı Devleti’nde Beşinci Kolera Pandemisi ve Sosyal Belediyeciliğin Salgının Önlenmesine Etkileri", Medeniyet ve Toplum Dergisi 8, no. 2 (2024): 294-298, Access February 8, 2026, https://dergipark.org.tr/tr/pub/metder/article/1610848.
[11]
John Snow, On the Mode of Communication of Cholera, 2nd ed. (London: John Churchill, 1855), 10-11, Access February 8, 2026, https://wellcomecollection.org/works/uqa27qrt/items.
[12]
Snow, On the Mode of Communication of Cholera, 68-75.
[13]
Aaron S. Bernstein ve Jonathan A. Patz, "Climate Change and Infectious Disease," in Harrison’s Principles of Internal Medicine, 22nd ed., ed. Joseph Loscalzo et al. (New York: McGraw Hill, 2022), 3748.

Historical Origins and Environmental Determinism
Atmospheric Conditions and the Influence of Winds
Water Sources and Local Temperament
The 19th Century ‘Sanitary’ Movement and Practices
Edwin Chadwick and the Sanitary Report
Florence Nightingale and Nursing Principles
Miasma Perception in the Ottoman Empire and the Case of Istanbul
The 1911 Cholera Outbreak and the Perception of “Air Change”
Social Municipalism and “Tebhir” Practices
Refutation of the Theory and Scientific Evidence
John Snow and Cholera Transmission
The Broad Street Pump and Water Supply Analysis
Modern Pathology and Contemporary Evaluation
Microbial Pathogenesis and Modes of Transmission
Reinterpretation of Environmental Factors