This article was automatically translated from the original Turkish version.
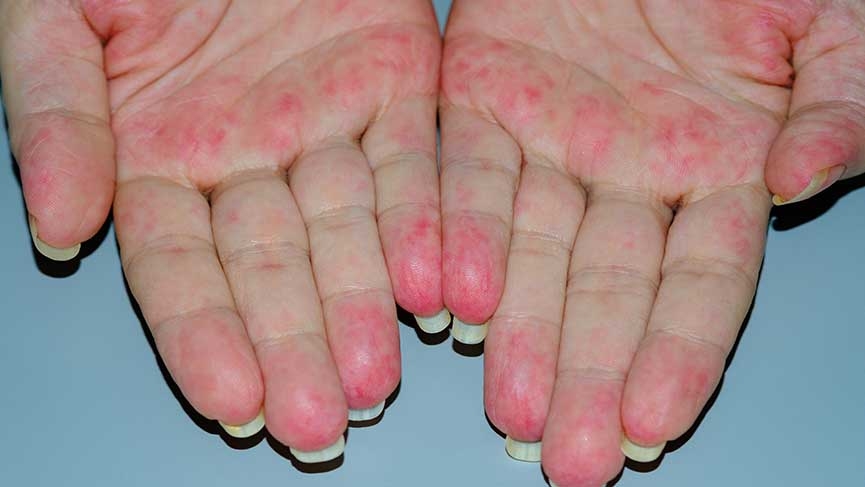
Cutaneous limited vasculitis is a form of vasculitis confined to the skin, classified as Cutaneous Vasculitis, Not Elsewhere Classified, small, characterized by inflammation of medium-sized blood vessels. Unlike systemic vasculitides, this situation affects only the skin and does not involve other organs. Cutaneous limited vasculitis typically presents with skin lesions such as palpable purpura, urticaria, vesicles or ulcers like. Although its etiology complete remains unexplained, it has been associated with various triggering factors including infections, drug reactions, autoimmune diseases and malignancies together.
Although cutaneous limited vasculitis can occur in any age group, it is more commonly observed in adults. It has a slightly higher incidence in women than in men. The exact prevalence is unknown, but most cases of cutaneous limited vasculitis are considered idiopathic. Risk factors include previous infections (particularly streptococcal infections), drug use (antibiotics, NSAIDs), chronic inflammatory diseases and malignancies.
Castaneous limited vasculitis is characterized by an inflammatory process initiated by the deposition of immune complexes in the walls of small vessels, leading to complement activation. This process results in vascular wall damage, leukocyte infiltration and ultimately tissue ischemia. The clinical findings in the skin reflect this inflammatory process. Pathophysiologic mechanisms include immune complex deposition, cytokine release and neutrophil activation important.
Castaneous limited vasculitis typically presents with palpable purpura, symmetrically distributed on the lower extremities (legs and foot ankles). Purpura consists of non-blanching, red-purple colorful skin lesions. Other clinical findings include urticaria, vesicles, bullae, necrosis and ulceration place. Lesions may be itchy or painful. Systemic symptoms (fire, fatigue, joint pain) are rare; their presence should prompt consideration of systemic vasculitis in the differential diagnosis.
The diagnosis of cutaneous limited vasculitis is based on clinical findings and histopathological examination. Skin biopsy is the gold standard for confirmation. Histopathology typically reveals leukocytoclastic vasculitis (neutrophil infiltration and fibrinoid necrosis of vessel walls). Laboratory tests aim to identify underlying causes. Tests may include complete blood count, erythrocyte sedimentation rate, C-reactive protein (CRP), antinuclear antibody (MAIN) and hepatitis serology.
Castaneous limited vasculitis may be confused with other forms of vasculitis and diseases causing cutaneous lesions. The following conditions should be considered in the differential diagnosis:
The treatment of cutaneous limited vasculitis depends on identifying the underlying cause and the severity of symptoms. In mild cases, symptomatic treatment may be sufficient. Nonsteroidal anti-inflammatory drugs (NSAIDs) and antihistamines are used to relieve itching and pain. In more severe cases, systemic corticosteroids (prednisone) or immunosuppressive agents (azathioprine, cyclosporine) may be required. If an underlying infection or drug reaction is identified, these conditions must be appropriately managed.

No Discussion Added Yet
Start discussion for "Vasculitis Limited to the Skin" article
Cutaneous Limited Vasculitis
Epidemiology and Risk Factors
Pathophysiology
Clinical Findings
Diagnosis
Differential Diagnosis
Treatment