This article was automatically translated from the original Turkish version.

Asthma is a chronic inflammatory respiratory disease characterized by reversible airway obstruction, excessive narrowing of the airways in response to various stimuli, and excessive mucus production in the airways. World According to data from the World Health Organization (WHO), it is a non-infectious disease affecting both children and adults and is the most common chronic disease of childhood. Although it can be controlled with proper management and treatment, it significantly impacts quality of life.
Both individual and environmental factors play important roles in the development of asthma. Individual factors include genetic predisposition as the most prominent. If there is a family history of asthma or allergic conditions, the risk of developing asthma increases. Atopy, or a tendency toward allergic reactions, may also contribute to asthma development. Hyperreactivity of the airways causes them to become overly sensitive to various triggers, thereby increasing asthma risk. Obesity is another factor that increases asthma risk by negatively affecting respiratory function. Additionally, asthma is more frequently observed in boys during childhood.
Environmental factors also play a significant role in asthma development. Allergens such as house dust mites, pollen, mold spores, pet dander, and cockroaches are common triggers. Viral respiratory infections, in particular, can sensitize the respiratory system and worsen asthma symptoms. Air pollution irritates the airways and increases asthma risk. Cigarette smoke, whether through active smoking or passive exposure, damages the respiratory tract and facilitates asthma development. Finally, stress is known to trigger asthma; under intense emotional stress, airway narrowing can lead to worsening of symptoms.
The foundation of asthma lies in chronic inflammation of the airways and the physiological changes it triggers. This process begins when the airways are exposed to triggers such as allergens, infections, or irritants. These stimuli activate immune cells, which then release inflammatory mediators such as histamine, leukotrienes, and cytokines. These mediators cause severe contraction of the bronchial smooth muscle (bronchospasm), leading to airway narrowing. Simultaneously, edema develops in the airway walls, and excessive mucus is secreted by submucosal glands.
This triple mechanism—bronchoconstriction, edema, and mucus accumulation—results in marked narrowing of the airways. This narrowing becomes critical during expiration (breathing out), as airways naturally narrow during this phase. In asthma, this narrowing is exaggerated, obstructing airflow. As a result, air becomes trapped in the alveoli (air trapping), and wheezing occurs. Impaired gas exchange leads to decreased blood oxygen levels (hypoxia) and carbon dioxide accumulation. The body compensates for hypoxia by increasing respiratory rate (tachypnea), but this can lead to respiratory muscle fatigue and metabolic acidosis. Chronic inflammation eventually causes structural changes in the airway walls. If untreated, this process accelerates disease progression and increases exacerbation frequency.
Diagnosis begins with a clinical evaluation. The patient’s history is assessed for recurrent breathlessness and nocturnal cough. During physical examination, wheezing is heard during moderate attacks, while silence over the chest may be detected during severe attacks. In patients with chronic asthma, an increase in the anterior-posterior diameter of the chest may be observed, and allergic conditions such as atopic dermatitis or eczema may coexist.
Laboratory tests also assist in diagnosis. Blood tests may reveal eosinophilia (greater than 5%) and elevated IgE levels. Sputum examination may show the presence of eosinophils. Skin prick tests (allergen tests) are used to evaluate the patient’s sensitivity to specific allergens. Pulmonary function tests are also essential. Spirometry, peak flow measurement, and bronchus provocation tests are used in diagnosis. Radiological imaging, including chest X-ray, is also performed. All these methods are evaluated together to establish a definitive diagnosis and determine appropriate treatment.

Before an attack, some early symptoms may appear. The individual may experience itching in the jaw and front of the neck, nasal congestion, and sneezing. As the attack begins, breathlessness and a sensation of chest tightness develop. A persistent, irritating, dry cough that worsens at night is a hallmark feature of the disease. Sticky, clear, frothy sputum may accompany the cough. Tachypnea (rapid breathing) and tachycardia (rapid heart rate) may occur. Exhalation duration is prolonged, and wheezing is often audible during this phase. The person gradually becomes pale, restless, and in severe cases, cyanosis (bluish discoloration of the skin and mucous membranes) may develop. Accessory respiratory muscles are recruited due to increased breathing difficulty. Sweating and excessive fatigue become prominent. As the attack worsens, speaking becomes difficult and may become impossible. Due to hypoxia (oxygen deficiency), loss of consciousness may occur, and the person may not respond even to painful stimuli.
The primary goal of asthma treatment is to control symptoms, prevent disease progression, and maintain quality of life. Both pharmacological treatment and lifestyle modifications are crucial in this process.
Pharmacological treatment is one of the cornerstones of asthma management: controller medications and reliever medications are the two main categories. Controller medications are taken regularly to achieve long-term control of the disease. They reduce airway inflammation and alleviate asthma symptoms. Reliever medications act rapidly and are used during acute attacks to quickly dilate the bronchi and ease breathing. If an asthma attack is triggered by an infection, antibiotics may be added to the treatment regimen. Asthma medications can be administered via different routes: oral, parenteral, and inhalation. Inhalation therapy is one of the most common methods in asthma because it delivers medication directly to the airways. Various devices are used in inhalation therapy. A nebulizer converts medication into a fine mist for direct inhalation. A metered-dose inhaler (MDI) can be used directly or with a spacer device to enhance drug delivery to the lungs. A dry powder inhaler (DPI) requires the patient to inhale forcefully to draw the medication into the airways and is primarily used for regular maintenance therapy.
Medication alone is insufficient to control asthma; preventive measures and lifestyle changes are also of great importance. Additionally, immunotherapy, which involves desensitization to specific allergens, can provide long-term benefits. For more severe cases, bronchial thermoplasty is an advanced treatment used to reduce airway hypersensitivity. In emergency situations, prompt intervention is essential. Educating families and children on how to respond during an attack facilitates early intervention and minimizes the impact of exacerbations.
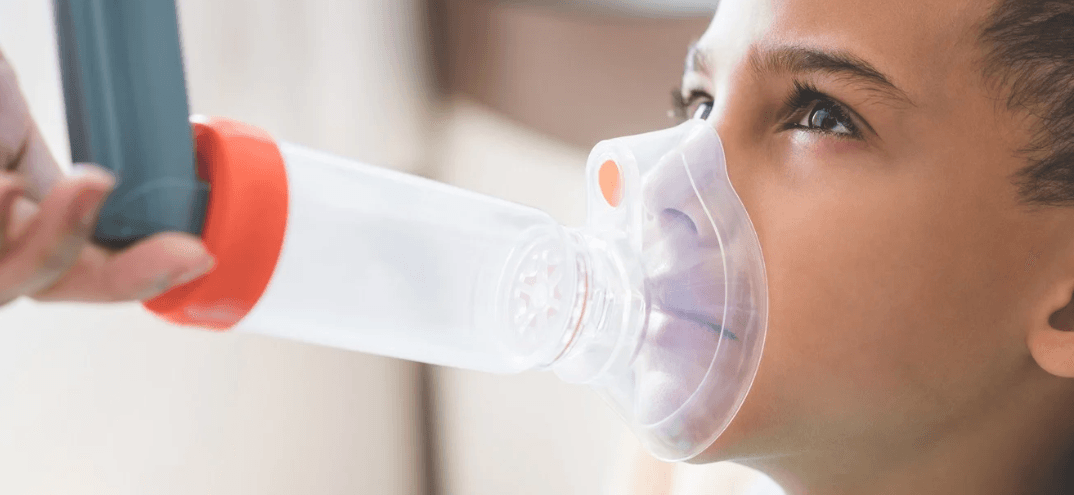
Family education is vital to maintaining the health and quality of life of a child with asthma. First, the disease, its diagnostic process, treatment methods, and medications must be well understood. Families must recognize early signs of an attack and protect their child from allergens that can trigger asthma. Foods that may provoke allergic reactions should be identified, and the child must avoid them. At the same time, exposure to high-risk environments should be avoided, and contact with sick individuals should be prevented. Breathing exercises support lung function and help the child cope with breathlessness. Daily activities and participation in sports should be encouraged within the child’s capacity to preserve both physical development and psychological well-being. The child should be encouraged to take responsibility for their own care and learn how to live with the condition. It must be remembered that stress can trigger asthma, and the child should be kept away from stress as much as possible. Furthermore, both family and child must be educated on how to use emergency medications during an attack.
The home environment is also of great importance in asthma control. Specific measures must be taken to control house dust mites. Unnecessary items and plants should not be kept in the child’s room, and cleaning should be performed regularly to prevent dust accumulation. Bedding, curtains, and pillow covers should be made of dust-mite-resistant fabrics and washed weekly at 55–60°C. Indoor humidity should be maintained below 50% because high humidity promotes mite proliferation. Avoiding keeping pets in the home will also reduce the risk of allergic reactions. With these measures, the child’s asthma symptoms can be controlled and their quality of life improved.

Etiology (Causes)
Pathophysiology (Mechanism of Development)
Diagnostic Methods
Signs and Symptoms
Treatment Approaches
Family and Patient Education